Rural Round-up: Rural Medical Generalism in Tasmania, Australia
– a different model may be required.
This month's rural round-up is written by a trio of Australians working in Tasmania, an oft forgotten part of Australia due to it being a separate island to the mainland. (Map sourced on Wikipedia)
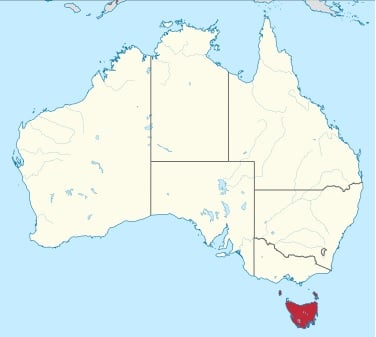
Tasmania is the Island State of Australia, lying in the Southern Ocean about 400 km south of Melbourne, between latitude 41 and 42. With a land mass of 91,000 km2, it is the smallest State, with a relatively static population of about 500,000, about half of them in the south in or near Hobart, the base for the State Government. Under the Australian Standard Geographical Classification – Remoteness Area (ASGC-RA) system, the whole State is regarded as regional, rural or remote, but the ASGA-RA system probably does not serve well the rather unusual Tasmanian context. Much of the land mass is rugged mountain terrain that is classified as a National Park, and there are both many scattered, small rural communities and genuinely remote communities, where access is restricted due to transport issues such as difficult road conditions (particularly in winter) and a lack of all-weather airports.
These smaller communities struggle to support resident medical practitioners, who often must work in sole practice situations. There are almost no acute hospital beds outside of the three major population centres and an entirely consultant-led hospital health service model. Rural general practitioners provide virtually no procedural care services. The peculiar demographics of the State make it difficult to develop a State-wide health system that provides equitable health care access for all residents.
As a result, the popular Rural Medical Generalist (RMG) pathway that originated in Queensland is difficult to translate into the Tasmanian context. While the local medical program at the University of Tasmania produces some graduates who want to be rural doctors, the well-developed Queensland RMG pathway is more attractive than the poorly coordinated approach in Tasmania. With no local employment opportunities, industrial awards or career structures for RMGs with additional procedural skills in anaesthetics, surgery and obstetrics, it is difficult to see how Tasmania can compete with the training pathways and career structures elsewhere in Australia.
This is not to say that Tasmania does not need RMG doctors with additional skills; the State clearly does. However, the additional skills need to be in other areas that are better aligned to the health care delivery model adopted by the State. There are many services that are under-represented in rural communities and could be incorporated into specific RMG training pathways and roles in the health care system. These include:
• Mental health;

• Palliative care;
• Chronic pain management;
• Care of the elderly;
• Child and adolescent health; and
• Emergency medicine in local community health facilities.
Photo: Tasmania - sometimes it snows .. one of the authors Dennis Pashen
There is also potential to develop a different workforce model in the North-West of the State, where there are two hospitals serving about 100,000 people living along a 150 km coastal strip. The current consultant-led model is struggling, because the population cannot support many consultants, who then become isolated and overworked, resulting in challenges in recruitment and retention. It may be more sustainable to employ a small number of consultants who act as resources to larger, self-supporting pools of RMGs with relevant procedural and other skills. This may produce a more stable and better supported group of practitioners who balance primary care roles with part-time specialist services, under the clinical supervision of consultants. In particular, the smaller of the two hospitals in the North-West – the Mersey general Hospital – may be an ideal location to establish RMG services, based on a small emergency department and a strong focus on elective surgery. Should this model be adopted, it would open up opportunities for RMGs with procedural skills to be both trained and employed in Tasmania as part of a State-wide health care system.
Tasmania has recently adopted a new model of health care delivery, based on a single, whole-of-State approach. A different model for the North West was included in discussions and consultations, but at this stage has not been adopted. There are community concerns about perceptions of reduced quality of such a model and political concerns about change management. However, we will try to keep the discussion alive, as there is no evidence to support concerns about quality and workforce challenges will continue in region. In the meantime, more work needs to be done to better define the non-procedural RMG roles and training pathways, better aligning the rural workforce to health care needs. It is possible that adoption of the Modified Monash model of rural classification will help by clearly separating the two major centres – Hobart and Launceston – from the rest of the State.
Richard Hays, Professor of Medical Education and Dean of Medicine, University of Tasmania
Dennis Pashen, President, Rural Doctors Association of Tasmania
Paul Fitzgerald, RMG Training Director
To read more about Rural Medical Generalism see the
Cairns Consensus 2013
or visit the website of the
Australian College of Rural and Remote Medicine