From the President: the whole is greater than the sum of its parts
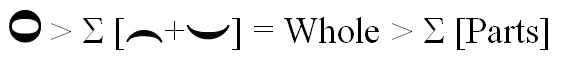
The whole is greater than the sum of its parts.
español
 Some truths need repeating, often using different language until we better understand. A recent meeting to plan a workshop for family doctors on multiple morbidities reminded me of this. Convened by the Dialogue on Diabetes and Depression (DDD), Prof Jan de Maeseneer hosted the planning session at the University of Ghent. The DDD is an international multi-disciplinary effort started in 2007 to improve the care and outcomes of those with both diabetes and depression. WONCA was a founding member of the DDD. The DDD plans to offer a series of workshops on diabetes and depression for diabetes specialists, family doctors and primary care workers, nurses, and mental health workers around the world.
Some truths need repeating, often using different language until we better understand. A recent meeting to plan a workshop for family doctors on multiple morbidities reminded me of this. Convened by the Dialogue on Diabetes and Depression (DDD), Prof Jan de Maeseneer hosted the planning session at the University of Ghent. The DDD is an international multi-disciplinary effort started in 2007 to improve the care and outcomes of those with both diabetes and depression. WONCA was a founding member of the DDD. The DDD plans to offer a series of workshops on diabetes and depression for diabetes specialists, family doctors and primary care workers, nurses, and mental health workers around the world.
Our task at the planning session was to develop the overall framework and goals for a family doctor workshop. We were a dozen experts from six countries. We represented behavioral health, diabetes, family medicine, internal medicine, nursing, psychiatry, and psychosomatic medicine. We reviewed the experience of the very first workshops on diabetes and depression that DDD conducted for nurses in Africa over the past year. We noted that the nurses preferred small group discussions that focused on local issues.
Encouraged by the success of the nurse workshops, we enthused that we would pioneer a new kind of thinking. We would solve the problem of fragmented care for those with multiple morbidities. We would begin by weaving several conditions into a single workshop that would be relevant to and centered on learners. We envisioned a future in which the multiple disciplines would bring their collective expertise together to address more effectively the comprehensive needs of the patient. We imagined that our workshops would stimulate interdisciplinary insights and cooperation to better serve the patient.
Then, reality set in. As we got into the details of exactly what the workshop should accomplish, it became obvious that we were speaking different languages. Our conflicts seemed to center around two key questions. Who should do what in the care of those with diabetes and depression or other multiple morbidities? What should be done to provide the best care for those with diabetes and depression or other multiple morbidities?
It seemed ironic that these basic questions could result in divergent opinions. How could such fundamental disagreement occur among bright, thoughtful, and well intended professionals? My service on more than three dozen national and international guideline panels has taught me that such conflicts arise with every guideline. My 30 years of practice experience has confirmed that such disagreements happen every day in practice. What follow are my reflections on ways to resolve these important disputes.
Who should do what versus what should be done
We each view the world through our own professional lens. We spend many years absorbing the language and culture of our respective disciplines. It is therefore understandable that those of us from a particular profession develop a uniform sense of what our roles are and should be in our various health care delivery systems. Thus, with every guideline we write and with every course we teach, we attempt to reinforce the idealized version of the role that we believe our profession should play in health care. Yet, our actual roles in the health system do not flow directly from our own perspectives and preferences. They are the result of the unique mix of resources, population needs, other professions, politics, and other competing forces that shape every health system.
An example is the declining role of cardiothoracic surgeons in the care of coronary artery disease (CAD). In the early days of interventional therapies for CAD, when coronary artery bypass graft surgery was the primary invasive treatment, surgeons dominated discussions on CAD therapy. The disruptive technology of angioplasty and stents changed that, with cardiologists becoming the dominant force in CAD treatment. The shrinking influence of surgeons in the management of CAD caused reductions in the number and economic power of those choosing cardiothoracic surgery as a profession. That is not the end of the story however, as surgeons respond to the changing and competitive landscape with their own innovations, such as minimally invasive surgery.1
We find proposals to limit or modify our roles as threats to our professional identity and to our livelihood. A substantial portion of meeting time for multidisciplinary groups consists of teaching other each what their group actually does, could do, and should do in the provision of health care. Consequently, we should expect that diverse groups of professionals will spend much of their time writing guidelines and developing courses in a power struggle for primacy.
If we turn to science as the dispassionate arbiter to resolve these professional disputes, we will be sorely disappointed. The science on what should be done for the individual patient is remarkably scant, almost shockingly inadequate. The science on who should do what is practically non-existent. From the point of view of the patient or the objective observer, these professional power struggles seem scientifically unwarranted and professionally self-serving. In the end, the needs of the patient and population are best served by coming to agreement on what should be done. After agreement is reached on what should be done, who should do it is often decided with less controversy.
What should be done, and who decides
Deciding what should be done can be very difficult. At a population level, our most influential studies produce findings that are accurate and enduring less than half the time.2 At the level of the individual patient, it is even worse. Unless the patient was actually enrolled in a study, we can never be certain that the study population’s demographics, setting, and findings are relevant for that particular patient.
Even more vexing is the challenge of coming to agreement on the outcomes that are viewed by the patient as most important. For example, while death is assumed to be an unwanted outcome, it is preferred by many to the outcome of a seriously disabling stroke.3 Especially disconcerting is the fact that decisions regarding the value of various outcomes are often left to those who specialize in a particular disease. Their expertise in a particular condition is assumed to confer expertise in the values and preferences of those with that disease, and that is often wrong.
One could just as easily argue that the ongoing relationship and more comprehensive knowledge of a specific patient place the family doctor in a better position to know the patient’s values and context. Too often, when trying to balance the competing views of a granular approach to a disease or a comprehensive approach to a patient, the more atomistic view prevails. This is because the more narrow perspective more likely provides the illusion of achievable precision (eg, get the hemoglobin A1c below 7% for 80% of those with diabetes), when contrasted against the less numerical aims of holistic care (e.g., respect people’s wishes to not have their lives revolve around a medical condition).
Additive versus substitutive or integrative
Once decisions are made as to what should be done, and who should do it, there remains the practical task of recommending how to best implement the decisions. Traditionally, such recommendations are additive rather than substitutive or integrative. In other words, when considering recommendations for best practices for those with both diabetes and depression, expert panels commonly add current recommendations for diabetes to those for depression. This often results in an impossibly long list of tasks to be accomplished in primary care that may not reflect patient values and may even conflict with one another (e.g., the treatment of diabetics with severe depression by using newer atypical anti-depressants, which may in turn worsen glucose control).
Conclusions
The most successful efforts to train family doctors in multiple morbidities will be mindful of several factors. What is acted on will inevitably be a reflection of professional biases and local circumstances. Science is often wanting when it comes to the care of an individual patient. Particular attention should be given to developing clinical recommendations that are integrative rather than additive.
Our planning group was able to arrive at a number of decisions. The first family doctor workshop will be in Ghent in October 2013. Its primary objective will be to improve the care and outcomes of those with multiple conditions, such as diabetes and depression. The workshop will promote a move from disease-oriented to goal-oriented care. Much of the workshop will consist of discussion among participants and invited patients, rather than lectures by narrowly focused experts. Small group sessions will train participants on how to empower patients to make better decisions and to develop skills at goal setting and shared decision making. Building on the success of the initial workshop, the plan is to conduct a number of similar workshops around the world in 2014 and beyond.
I learned several important lessons at the planning session. I learned that we need a new paradigm when it comes to caring for those with multiple morbidities. We need to think more about goals and less about disease. We need to develop better skills in helping people identify and accomplish their goals. As our thinking changes, our language will change. We will move from the language of disease, such as the International Classification of Disease (ICD), to the language of goals and function, such as the International Classification of Function (ICF). I also re-learned an enduring truth: that the whole is greater than the sum of its parts.
Professor Richard Roberts
President
World Organization of Family Doctors
References
1. Mathiesen DJ. Is it an opportune time to be interested in cardiothoracic surgery?
http://aats.org/TSR/Cardiothoracic-Surgeon/Interested-in-cardiothoracic-surgery.cgi
2. Ioannidis JPA. Contradicted and initially stronger effects in highly cited clinical research.
JAMA. 2005;294(2):218-228. doi:10.1001/jama.294.2.21.
3. Solomon NA, Glick HA, Russo CJ, Lee J, Schulman KA. Patient preferences for stroke outcomes. Stroke 1994 Sep;25(9):1721-5.