From the President: The World Bank, Romania & ICPC… read on
 español
español
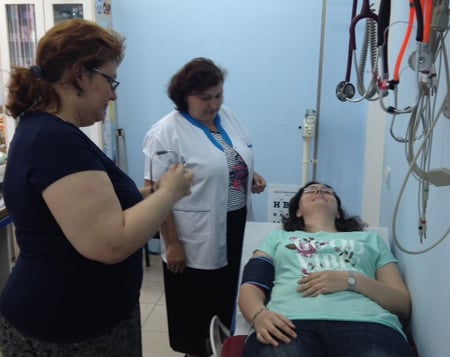
Dr Sandra Alexiu is a family doctor in Romania, and a member of WONCA’s working party on rural practice. Sandra practices in a small community called Jilava, outside the capital city of Bucharest. Sandra works in partnership with a primary care nurse, and together they provide care to a population of 2,500 people.
Photo: Rural family doctor, Sandra Alexiu (left), at her family practice clinic in the small rural community of Jilava in Romania
In Romania family medicine is a recognized specialty, with three years of required postgraduate training and formal assessment at the end of training. Like several other countries in Eastern Europe, Romania reformed its health care system, based on family medicine and strong primary health care, about 20 years ago, in order to ensure that all people have access to high quality community-based health care.
More than 45% of Romania’s population of 20,000,000 live in rural areas, and, as in many other parts of the world, it is family doctors like Sandra who are usually the only doctors serving rural communities.
 Photo: Romanian Health Minister Nico Baniciou meets WONCA President, Professor
Michael Kidd, and World Psychiatric Association leaders including
President Dinesh Bhugra
Photo: Romanian Health Minister Nico Baniciou meets WONCA President, Professor
Michael Kidd, and World Psychiatric Association leaders including
President Dinesh Bhugra
I was in Romania in June to deliver the opening address at the 2015 World Psychiatric Association Congress, held in Bucharest. The conference had a special focus on the integration of mental health into primary care. A copy of my address is
available here.

The visit provided me with the opportunity to meet with Sandra and other family medicine colleagues in Romania and to discuss some of the challenges facing family medicine and the delivery of universal health coverage. Dr Rodica Tanasescu, president of WONCA’s member organization in Romania, the National Society of Family Medicine, told me that there is a continuing challenge to define the role of the family doctor, and the required postgraduate training curriculum, in the face of what feels like endless rounds of health system reform. I was advised that Romania has had 24 health ministers in the 25 years since the end of Communism, each with their own ideas on health reform and the place of family medicine. In the meantime the nation’s dedicated family doctors continue to deal with the challenges and uncertainty, and provide the best care they can, often with inadequate support and resources.
Photo: Dr Rodica Tanasescu and other leaders of Romania’s National Society of Family Medicine at the Society’s offices in Bucharest
Romania, like most countries, is seeking to strengthen the nation’s primary health care system in order to best meet the needs of their population and ensure universal health coverage. The delivery of universal health coverage will receive global attention in September 2015, when the United Nations adopts the new Sustainable Development Goals for 2015-2030. Nations will be looking for ways to measure whether they are meeting these new global development goals.
The World Bank, the Bill and Melinda Gates Foundation, and the World Health Organization (WHO) have established the new Primary Health Care Performance Initiative (PHCPI) to encourage countries, especially low and middle income countries, to achieve universal health coverage, by supporting improvements in each nation’s primary health care system, through better measurement, knowledge-sharing of best practices, and the provision of practical tools to manage and improve delivery of essential health services.
 Photo: Palace of the Parliament, Bucharest, Romania
Photo: Palace of the Parliament, Bucharest, Romania
WONCA has been asked to assist the World Bank, the Gates Foundation and the WHO in the development of these measures of primary care effectiveness. In June I was invited, as president of WONCA, to contribute to a meeting about the new Primary Health Care Performance Initiative, held at the World Bank Headquarters in Washington DC.
It is clear that to date attention appears to have been on “what we can measure, rather than on what we should be measuring”. I see this as the fundamental challenge that will determine whether this initiative delivers real improvements in global primary health care. We should not be limited by current data sets as these largely focus on vertical program delivery.
Part of the challenge facing this Initiative is that the funders describe primary care as a “Black Box”. A “Black Box” is something that can be viewed in terms of its inputs and outputs without any knowledge of its internal workings. I am troubled that our work in primary care is seen as a “Black Box”. The work we do may seem impenetrable to health care policy makers and statisticians who haven’t engaged closely with us, but those of us working inside the “Black Box” see everyday the benefits of the work that we do with our patients and with our communities, and we understand the workings very well.
Primary care is a complex system, just like hospital-based health care, and is no more a “Black Box” than hospital-based health care. But what makes primary care more difficult to understand and measure are the added challenges of care delivery being distributed, rather than centralized, of being delivered by multiple types of health care providers, often with a mix of private and publicly-funded services with patients moving between providers, and with a lack of standardized ways to capture data about what we actually do.
WONCA recognized many years ago that we would not see the improvements we wanted to see in primary care unless we could measure what was happening in our clinics, and this required a standard system of coding and classification. This led to the development of WONCA’s International Classification of Primary Care (ICPC), now part of the World Health Organization’s Family of International Classifications. ICPC is used in many countries, including low and middle-income nations. Importantly ICPC does not just record the diagnoses made in primary care, but also allows us to record the Reasons for Encounter, the reasons why someone has presented to our clinic, and so allow us to capture details of our patients’ symptoms and signs and allow us to examine health-seeking behaviours in different contexts. ICPC also allows us to record what happens following a consultation, through referrals to consultant specialist services, ordering of investigations and ordering of medications, which allows measurement of flow-on costs throughout the rest of the health system, and the targeting of education to support the efficient and effective use of limited health resources.
I am pleased to see that the vital sign indicators of new Primary Health Care Performance Initiative do not just include vertical disease-focused measurements, but also include important health system indicators that provide some indication of how well a nation’s primary health care system is working. This includes measures of primary health care expenditure as a proportion of a nation’s total health expenditure. This needs to be expanded to measure appropriate spending, especially on those activities that genuinely knit primary health care interventions together.
The new Primary Health Care Performance Initiative also includes a number of condition-specific health outcome measures and, while these are important indicators of specific health improvements, the risk of focusing on these alone is that policy makers and funders will continue to pursue vertically-oriented approaches to health care, rather than focus on much needed health system strengthening measures.
I was asked by the World Bank and Gates Foundation to outline the sorts of measures that can demonstrate how well we integrate vertical programs into existing health systems to create primary care-led health systems.
For example, it is important to be able to measure where our primary care clinics are based, compared to the population. And particularly to measure whether we are meeting the needs of those communities in greatest need, including people who are poor or otherwise disadvantaged and marginalised, and especially those based in rural and remote locations.
Similarly measuring the staffing profile in primary care is important and needs to include family doctors as well as community health workers, primary care nurses, midwives and birthing attendants. It is a mistake to think that people in low and middle-income nation don’t want and deserve access to caring and competent primary care doctors. The presence of a doctor can turn around unfavourable local community attitudes towards a community health service and improve the quality and range of services on offer.
We need measures of the percentage of the graduating output of the nursing schools and medical schools in each country who are destined to work in the community in primary care. For doctors, WONCA believes this needs to be around 50% of all medical graduates if health systems are going to be sustainable and equitable. Too many countries are training too many hospital-based medical specialists at the expense of strengthening their primary care medical workforce, with the attendant diversion of health spending away from the community where it is most needed.
 Photo: Typical pharmacy in Romania
Photo: Typical pharmacy in Romania
We also need measures of whether a country values health care professionals who work in primary care. Is family medicine recognized as a medical specialty? Do doctors require supervised postgraduate training before being released to work in primary care? Do we send our most experienced doctors and nurses to work in the most challenging health care settings, in remote rural locations and with disadvantaged communities, or do we send recent medical and nursing graduates with no clinical experience and inadequate supervision? Are there opportunities for career advancement for those working in primary care? Are suitable clinic facilities provided to allow clinicians to use their skills and training to deliver the best quality care? And do nurses and doctors working in primary care, especially in remote rural areas, receive higher incomes that nurses and doctors working in hospitals? I use an index to compare countries called the “Health Minister’s Salary Index”. Does a family doctor working in a remote rural area receive a higher salary than the nation’s Minister of Health? It seems to me that if a nation is paying its health care professionals working in the most challenging circumstances more than their politicians, they are probably on the right track.
One of the great challenges of universal health coverage is how do we adopt true person-centredness into our health services. We need to be able to measure person-centredness through indicators such as patient satisfaction, access to care after hours, access to home-based care, measures of continuity of care, access to interpreters, physical access to our clinics and services for those with a disability, and the integration of preventive care and health promotion services into primary care services. We also need to include measures of quality and safety in primary care, such as infection control, vaccine cold chain compliance, and our preparedness for epidemics of infectious diseases.

The so-called gatekeeper role of primary care providers is also important. Do people need to attend primary care before they can access expensive specialist consultant services and investigations? The gatekeeper role is an effective way to contain a nation’s health care costs, prevent unnecessary expenses for patients and their families, and tackle the challenges of overinvestigation and overmedication and potential iatrogenic harm.
Photo: A stork resting on a typical small church in a village in Romania’s Danube Delta region
These are all measures that indicate whether or not a nation values primary care and whether each nation genuinely sees primary care as the best way to ensure universal health coverage and improve the health and well being of their entire population.
Whether we like indicators or not, the Primary Health Care Performance Initiative of the World Bank and the Gates Foundation will be an important part of global primary health care development over the years ahead. It also provides a real opportunity for WONCA to work with other major global organisations to improve the quality of life of the peoples of the world through fostering high standards of care in family medicine.
Michael Kidd
WONCA President